IBS & THE BRAIN
Why it's all in your head is both wrong & right

"There's No Such Thing As The Mind-Gut Connection"
Recently, someone in an IBS support group on Facebook claimed there's no such thing as a mind-gut connection.
Wow. Let me be very blunt before we get into the science.
• Why do humans and animals shit themselves when they're terrified?
• Why do people, about to do something nerve-wracking, get butterflies in their stomachs?
• Why can someone watching something gory on TV throw up?
Now, I get why someone might think there's no connection. It's understandable. Hearing it's "all in your head" or "it's just stress" when a sufferer experiences very real physical symptoms can make some push back against the idea that it's psychological.
But, here's the problem
The mind-gut connection isn't alternative medicine, and it's definitely not saying your symptoms are imaginary.
It's a well-documented physiological system known as the gut-brain axis, and it plays a major role in IBS
Understanding it properly may actually give you more control, not less.
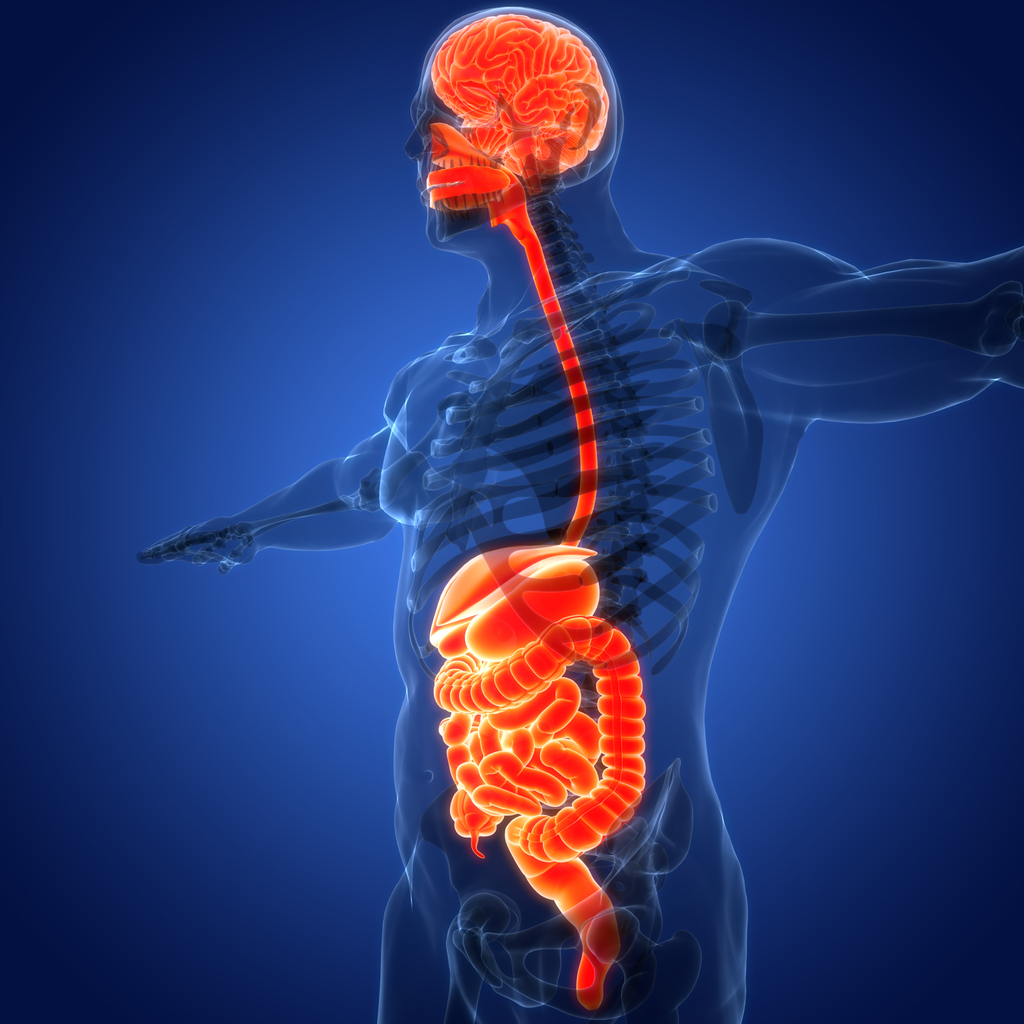
So, What Is The Mind-Gut Connection?
The technical term is the gut-brain axis
It refers to the constant, two-way communication between your digestive system and your brain.
This communication happens through:
The Autonomic Nervous System
The Immune System
Hormones
The Microbiome
And, Most Importantly, The Vagus Nerve
Your gut also contains its own complex neural network called the enteric nervous system. It contains over 100 million nerve cells.
This is why, recently, some started to refer to the gut as "the second brain."
That's not metaphorical, and it's not pseudoscience. It's anatomy.
Signals travel from the brain to the gut, and from the gut to the brain, in a continuous loop
Your gut can influence mood, and your brain can influence motility (muscle contraction in the GI tract), pain perception, inflammation, and secretion.
IBS Is Real
And It's Neurological As Much As Gastrointestinal
Let's clear up a few things before we move on.
IBS Is NOT Imagined
IBS is NOT Weakness
IBS is NOT A Character Flaw
Major medical organizations, including the American College of Gastroenterology and the National Institute of Diabetes and Digestive and Kidney Diseases, recognize IBS as a legitimate disorder involving abnormal gut-brain interaction.
One of the defining features of IBS is visceral hypersensitivity.
That simply means your nervous system processes normal digestive activity as painful or urgent.
The same gas that wouldn't bother one person can trigger severe discomfort in someone with IBS.
That isn't imaginary!
That's altered neural processing.
Functional MRI studies show that people with IBS demonstrate different patterns of brain activation in response to gut stimulation compared to those without IBS
Different wiring. Different amplification
That's neuroscience
How Stress Actually Affects The Gut
This is where people get defensive
When doctors say, "stress plays a role," patients hear...
"You're anxious."
"You're being dramatic."
"You need to calm down."
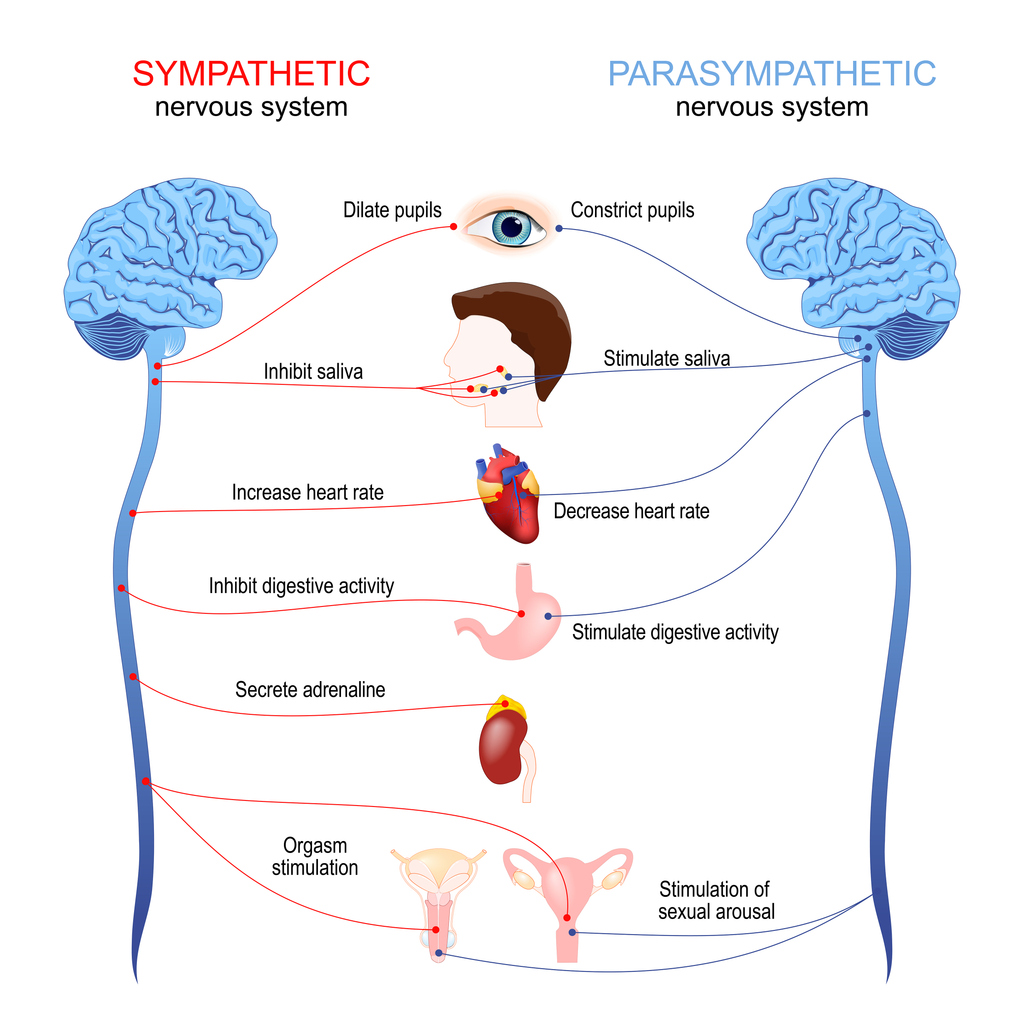
But that's not what stress means physiologically. Stress activates the sympathetic nervous system, or what you might know as the fight, flight, or freeze response.
When that system activates:
• Gut motility changes
• Blood flow shifts
• Inflammation can increase
• Pain sensitivity rises
• Gut permeability may change
So, stress doesn't create IBS out of thin air. But, in someone predisposed to IBS, it can certainly amplify symptoms significantly.
And here's something else.
Just as stress can trigger the gut, the gut can also trigger the stress response!
If your digestive system becomes unpredictable, your brain can become hypervigilant. That hypervigilance increases sympathetic activation, which in turn makes the symptoms worse.
That's a vicious cycle for a sufferer.
The Microbiome:
Your Gut Bacteria And Mood
Fortunately, research over the past 15 years has expanded dramatically in this field.
Your gut bacteria produce and regulate neurotransmitters like serotonin and GABA.
In fact, a large percentage of serotonin in the body is produced in the gut.
Publications from institutions like Harvard Medical have discussed how microbiome imbalances may influence anxiety, depression, and stress reactivity.
That means the communication is definitely not one-way
The brain affects the gut
The gut affects the brain.
Why The Phrase Triggers Some
Now, I don't know if the person who attacked the poster who mentioned the gut-brain connection was just ignorant or triggered.
But I do know some people don't like the idea, because in their minds, it sounds like blame.
Historically, IBS patients were dismissed. If a colonoscopy looked normal, patients were told, "There's nothing wrong with you."
So, when someone hears "brain involvement," they think "They're saying I made this up."
But involvement is not invention. If you touch a hot stove, your brain processes pain. That doesn't mean the burn is imaginary.
Similarly, IBS pain involves altered pain processing.
What This Means For Treatment
Here's where things get interesting, and empowering
If IBS involves abnormal gut-brain signaling, then treatment can target things like:
• Diet
• Microbiome
• Inflammation
• Motility
• AND nervous system regulation (which is where I, as a hypnotist, come in)
Major guidelines, including those from the National Institute for Health & Care Excellence, include psychological therapies such as CBT and hypnosis as evidence-based treatments for IBS.
Not because IBS is imaginary, but because the nervous system is part of the disorder.
Brain-based interventions can:
• Reduce pain sensitivity
• Normalize gut motility
• Reduce Urgency
• Decrease Symptom Flare Frequency
This isn't positive thinking woo-woo. It's nervous system modulation which is one area in which hypnosis shines.
Brain Imaging Studies In IBS
Functional MRI research has shown that IBS patients often exhibit increased activity in brain regions associated with:
• Pain Perception
• Emotional Regulation
• Threat Detection
In simple terms, the alarm system is more sensitive in IBS patients
When a normal digestive correction occurs, the brain may interpret it is as dangerous or urgent.
That's central sensitization, and central sensitization is treatable.
Common Objections
"If It's Stress, Why Do I Get Diarrhea?
Because stress affects motility. The autonomic nervous system directly influences how fast the gut moves
"Why Do Antibiotics Sometimes Help?"
Because they affect the microbiome, another component of the gut-brain axis.
"Why Do Symptoms Flare Before Big Events?"
Because anticipatory anxiety activates the sympathetic nervous system before the event even starts.
That's not weakness, it's just wiring.
Wrapping Up
So, IBS is not "all in the gut," and it isn't "all in your head."
It's the communication between the two.
Ignoring the brain leaves half the system untreated, and ignoring the gut does the same.
The most effective approach is integrated, or, as I like to tell the physicians I collaborate with, "You work on them from the neck down, and I'll work on them from the neck up."
FAQ
Is The Mind-Gut Connection Real?
Yes, absolutely. The gut-brain axis is a scientifically documented communication network between the brain and digestive system. It involves the autonomic nervous system, immune signaling, hormones, the microbiome, and the Vagus nerve.
Major medical organizations recognize abnormal gut-brain interaction as a core feature of IBS.
Is IBS All In Your Head?
No. IBS is a real gastrointestinal disorder. However, the brain plays a role in how pain and digestive signals are processed. In IBS, the nervous system can become hypersensitive, amplifying normal digestive activity into discomfort or urgency. That does not mean symptoms are imagined.
How Does Stress Affect IBS Symptoms?
Stress activates the sympathetic nervous system, which can alter gut motility, increase pain sensitivity, and change digestive function. For people with IBS, stress can significantly worsen symptoms due to the two-way communication within the gut-brain axis.
Can Hypnosis Help With IBS?
Gut-directed hypnosis has been studied as a treatment for IBS and is included in treatment guidelines in certain countries. It works by helping regulate nervous system responses and reducing visceral hypersensitivity.
Hypnosis does not "cure" IBS, but it may reduce symptom severity and flare frequency in some individuals.
What Is Gut-Directed Hypnosis?
Gut-directed hypnosis is a structured approach that focuses on calming the nervous system and improving communication along the gut-brain axis. It aims to reduce pain sensitivity, urgency, and stress-related flare-ups.
Is hypnosis for IBS Available In The Lake Norman Area?
Yes. At Hypnotic Shift in Cornelius, North Carolina, sessions are available for clients in Lake Norman, including Huntersville, Davidson, Mooresville, Denver, Charlotte, and surrounding areas.
Sessions are also available via Zoom for clients
Can I Get Help With IBS Over Zoom Or Online?
Yes. Online sessions can be especially helpful for people with IBS. Many sufferers experience anxiety about travel, long car rides, or being away from the restroom during flare-ups. Working from home removes that pressure.
Online sessions allow you to stay in a familiar, comfortable environment, which can actually support nervous system regulation.
How Many Sessions Are Needed For IBS?
We have found five sessions spread over 8 to 10 weeks to be the most effective.
Should Hypnosis Replace Medical Treatment For IBS?
No. Hypnosis should complement, not replace, appropriate medical evaluation. IBS should first be diagnosed properly by a healthcare professional to rule out other conditions.

